Vaccination
The coronavirus pandemic has caused our public spaces to shut down. The economy has stopped, we’ve socially distanced from our loved ones, and we may not get back to normal until there’s a vaccine. Could the extremity of this situation lead vaccine dissenters to change their minds about the benefits of vaccination?
Bernice Hausman leads the Department of Humanities at the Penn State College of Medicine, where she researches the history and meaning of anti-vaccination sentiment. She’s interested in medical controversies that spill over into the public realm, becoming social controversies. “It’s this interface between science and society,” she says, “which means you’re working with culture and tradition and ritual and history — not just with science.”
In order to understand why skepticism about vaccines is so durable, you have to understand the long history of anti-vaccination movements in the U.S., and how they connect to very big ideas about individual freedom and state power.
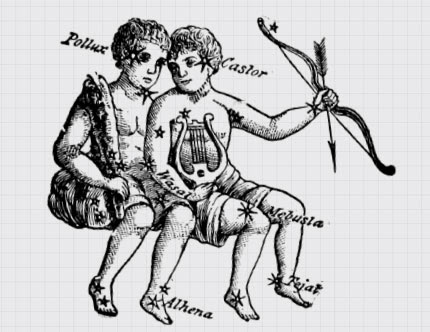
The earliest method of immunization, which dates back to the 10th century, was something called variolation* and it was used to protect people against smallpox. Variolation involved collecting matter from active smallpox lesions and then scraping it into the arms of people who weren’t ill. The idea was that hopefully, a mild, protective infection would result.
*IMAGE SEARCH OF “VARIOLATION” NOT RECOMMENDED.

Variolation eventually spread from China and India, where it originated, to the west, where the practice gave way to vaccination. In the late 1700s, an English physician named Edward Jenner made a vaccine for smallpox that was based on cowpox, a related animal infection. And while many people welcomed the new vaccines that began to develop from that point forward, there were also objections, right from the start. “Some of them based on the notion that… it’s always dangerous to mess around with nature, and people who do so are punished,” cites Hausman. “There were some anti-scientific arguments based on the notion that naturally becoming ill was preferable to being vaccinated. There were perceptions about the danger of vaccination. So all of the same concerns that we see today in contemporary vaccination dissent, you can see them historically.”
A big sticking point for a lot of people was vaccine mandates. Great Britain implemented compulsory vaccination in the mid-1800s and people rioted in response.

Print (color engraving) published June 12, 1802, by H. Humphrey, St. James’s Street.
Vaccine dissenters believed the government should not be telling people what to do with their bodies— and that was especially true if there might be even a small amount of danger involved. “What you tend to see, in the United States at least, is a mingling of arguments about freedom and individual rights with the notion of bodily danger,” says Hausman.
Hausman traces the modern anti-vaccination movement to the 1970s when parents started to express concerns about the original pertussis vaccine, which caused high fevers and febrile seizures in some children. “There was an increasing belief that it could cause some neurological damage,” says Hausman.
In the early 80s, a TV news program called Vaccine Roulette highlighted the growing controversy. In general, the program emphasized the risks of the vaccine while minimizing the dangers of the actual disease. Some of its more serious claims have been debunked by further research. The story also provided a big platform for a group called Dissatisfied Parents Together, which would go on to become the National Vaccine Information Center — which is now one of the biggest self-styled “vaccine safety” organizations in the country.
Another example of a single article having outsized influence is Andrew Wakefield’s fraudulent paper linking the MMR vaccine and autism, published in 1998. His findings have since been disproven many times over. There is no link between MMR and autism. But the association remains stubbornly persistent and still motivates some vaccine refusal.
Today, Dr. Hausman is observing and formulating some questions that might be interesting to investigate. She says this is an unprecedented time to be studying attitudes about vaccination because we’re in the midst of the first worldwide pandemic of the vaccine era.
As she watches anti-vaccination communities and messaging from organizations like the National Vaccine Information Center, she’s seeing a lot of fear among more ideological anti-vaxxers. People are watching the government enact stay-at-home orders and they’re worrying that it might lead to other heavy-handed government action. They worry about the possibility of more tightly enforced vaccine mandates and a crack-down on exemptions.
But Dr. Hausman also predicts that the pandemic may influence the views of those who are more “vaccine-hesitant,” leading them to embrace vaccination when they may not have before.
She’s also keeping an eye on the development of one potential coronavirus vaccine, which is being developed at the University of Pittsburgh. It takes the form of a patch, not an injection. It’s placed on the skin like a band-aid and over the course of a few days, it delivers the vaccine through a number of tiny needles. “Think about what it would mean if you went to the doctor’s office and instead of giving your child shots, they gave you four patches,” she says. The patient could administer them over a number of weeks, watching to see if their child had an adverse reaction to any of them. “You’re more in control as a parent. Even if it’s the same delivery of the same vaccines, it changes your relationship to the whole process.” She’s curious if the mechanism of delivery might change patient attitudes about vaccination.
Ultimately, what Hausman is seeing at this moment displays the same dynamics we’ve seen over and over again in history. Even when there’s overwhelming scientific evidence that vaccines are a good thing for public health, it doesn’t necessarily mean everyone just gets on board.

Comments (6)
Share
“A sable cloud turns forth its silver lining on the night.”
First, thank you for the episode. I enjoyed it very much. But my neuroticism compels me…
I understand the desire to avoid aggrandizing anything about the pandemic, but man it bugs the hell out of me that the phrase silver lining has become a virtual persona non grata in the language of the day. It’s well-intentioned, but semantically misguided, conflating the meaning of the phrase with something more akin to blessing in disguise. The key here is that claiming a silver lining entails no transmutation or elevation of the central object.
It would be repugnant to describe covid-19 as a blessing in disguise, obviously. But it is entirely appropriate and not at all insensitive to call the oceanic silence for the whales in Glacier Bay or the relatively clean air in India’s cities a silver lining to covid-19, or more precisely to the shelter-in-place response to cover-19. That’s precisely what those things are and it does not glorify the disease to say so.
Hoping there will be a follow up story on the humpback whale study
I enjoy this podcast so much!
Just after listening to this podcast, I saw this article about a leading anti-vacer in a video describing COVID-19 as a corrupt scheme / hoax being perpetrated on the world. Just as described, many are doubling down on their anti-science, conspiracy laden beliefs.
The “Plandemic” Video Has Exploded Online — And It Is Filled With Falsehoods https://www.buzzfeednews.com/article/janelytvynenko/coronavirus-plandemic-viral-harmful-fauci-mikovits
Love 99%!!!
Surely, boredom is being obliged to do something don’t want to do or, looked at another way, having nothing to do that you want to do.
Anything over 300 on the air quality scale is dangerous. We’ve had 2 years in the last 4 that have had that level in Spokane WA. I have a friend that lived in Indonesia and she said 900 is like sticking your face in the smoke from a campfire.
Very interesting episode!
However, as someone who visited Beijing in 2008 and then lived there full time from 2009 until 2018, this power-of-the-people conception of improvements in air quality is 99% false. The story gives the impression that the glimpse of blue during the Olympics led to widespread pressure from citizens and subsequent policy changes to address air pollution.
In reality, the government continued to publicly deny air pollution readings in Beijing until the heavily polluted winter of 2013. Between the Olympics and that moment (about 4.5 years), there were no significant changes in air quality or how most people dealt with “the fog”. It’s quite possible that air pollution actually got worse due to increasing electricity consumption, non-stop construction and the ever growing appetite for cars. Until 2013, air purifiers were outrageously expensive and almost exclusively imported machines owned primarily by expats. Proper masks on polluted days were also something you pretty much only saw on expats. Expats, it should be noted, make up an incredibly small fraction of the city’s population. Based on my own experiences, I had the feeling that the overwhelming majority of Beijing citizens didn’t have a clear conception of the pollution problem.
But after that admission by the government in the winter of 2013, all of a sudden air filters were sold out across the city and, much like the current coronavirus situation, N95 masks immediately became rare and coveted jewels. Despite the public’s awareness at that point, it was probably another 2 or 3 years after that until significant and sustained improvements in air quality came about.
The whole thing, and I think a large number of experts on Chinese policy would agree, is more of a numbers game than a reaction to public opinion. The government supported the continuation of horrendous pollution because those tiny air particles represented cheap economic growth. When the drawbacks (health problems, decreased productivity, poor international image) started to outweigh the economic benefits, then strong measures were taken to get to the point where Beijing is today.
India might end up being a different story after this current streak of blue skies because of obvious differences with China in terms of governance. But anyway, the story of Beijing as it was portrayed in the episode, even though it makes the episode tidier, felt quite inaccurate to me and I thought that I should offer this more nuanced version from someone who lived through it.